Stories
The Future of Healthcare is Less Invasive
The COVID-19 pandemic has forced hospitals to deal with the conflicting demands of clearing surgical backlogs and creating inpatient bed capacity. Minimally invasive surgeries can be part of the solution to help lower wait times.
One of the greatest lessons the pandemic has taught us is that we need to prioritize solutions that free up bed capacity and reduce the burden on healthcare professionals, while also reducing the risk of virus and infection exposure to both clinicians and patients. We can do this by leveraging technologies and processes that reduce the time between procedures and discharge, prevent readmissions, and allow for remote monitoring from home.
How? By expanding the use of minimally invasive surgeries (MIS).
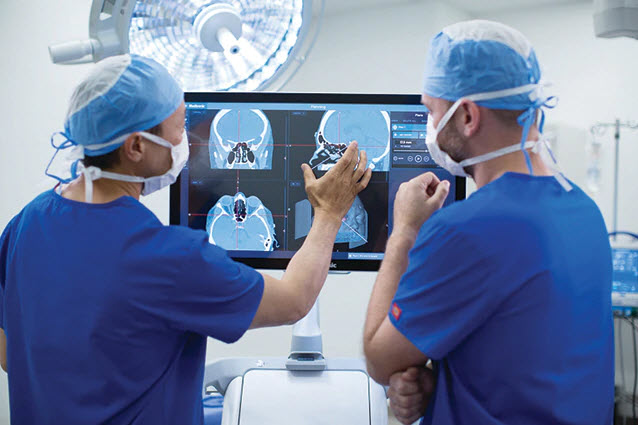
Expanding use of MIS
When compared to open surgery, MIS patients can experience lower rates of complications, shorter hospital stays, decreased blood loss and lower readmittance rates – all at lower overall cost[1]. In addition to traditional MIS procedures, MIS can be further leveraged and expanded through minimally invasive implants, robotics and virtual care.
Consider how miniaturization innovations in pacemaker technology have enabled some cardiac patients to avoid more invasive surgery through a minimally invasive procedure by replacing a traditional pacemaker with a tiny leadless, capsule-shaped device – approximately 2.5 centimetres in length – that is implanted directly into a patient’s heart via a catheter through the femoral artery. Or the transcatheter aortic valve implant that can also be implanted via a catheter, avoiding the higher risk of complications associated with major open heart surgery.
Wait lists for diagnostic and surgical procedures delayed due to the pandemic are estimated by Deloitte to be over 300,000 procedures in Canada.
Robots can help reduce risk
Paired with Robotic Assisted Surgeries (RAS), the benefits of MIS can be further amplified. Robotic surgery allows surgeons to conduct procedures through even smaller incisions which reduce recovery time and risk of infection. For example, a 2019 study in Denmark comparing minimally invasive RAS for endometrial cancer found the use of minimally invasive RAS reduces surgical morbidity and significantly reduced risk of severe complications.
In highly complex surgeries, such as spine surgery, RAS enables increased accuracy and precision resulting in reduced operative time, length of stay and blood loss, as well as providing a less disruptive option to the patient.
Leveraging collective will
This change to increased use of minimally invasive surgeries, supported by robotics, can be achieved faster than most would think. The example of increased utilization of virtual care in 2020 is proof of what’s possible when there is a collective will to implement solutions with a clear benefit to patients, healthcare providers, and the healthcare system.
The use of remote monitoring technologies for people with Type 1 diabetes and cardiac patients with implanted devices has increased significantly during the pandemic for these reasons. And numerous studies have demonstrated that remote monitoring of cardiac device patients can reduce in-person clinic visits with no change in patient safety[i]

Patient Preference
Patient preference for virtual care during the pandemic made adoption easier. The same can be expected of minimally invasive surgery. We need to begin to see patients as consumers and rethink care from their perspective, offering procedures that minimize not only their exposure risk but also their discomfort and the disruption of their daily life.
We are in desperate need for innovative solutions to overcome the destructive impact COVID-19 has had on our healthcare system. There has never been a better time to harness the full power of minimally invasive surgeries.
Reprinted with kind permission from Hospital News
REFERENCE
1 Sadri, H. (2020) Breaking Down the Silos: Transcatheter Aortic Valve Implant Versus Open Heart Surgery